New Law on DOT Physical Sleep Apnea: What You Need to Know
With the recent implementation of new regulations concerning DOT physical sleep apnea, understanding how these changes affect health and safety is crucial. For those dealing with issues like sleep apnea brain damage or coping with sleep apnea brain fog, staying informed on the latest requirements can lead to better health outcomes.
These laws aim to address concerns about sleep apnea brain damage and its potential effects on driving safety. By understanding the link between sleep apnea and issues such as sleep apnea memory loss, drivers can take proactive steps to manage their condition effectively.
Understanding the New Law on DOT Physical Sleep Apnea
What the Law Means for Drivers
The new law on DOT physical sleep apnea encompasses guidelines that require drivers to undergo thorough evaluations. These assessments are intended to ensure that those behind the wheel are not impaired by conditions that could affect their vigilance and reaction times. Partial compliance and regular check-ups are strongly encouraged.
For drivers, this means that if they exhibit symptoms of sleep apnea, such as excessive daytime sleepiness or snoring, they may be required to undergo a sleep study. The results of these studies can significantly impact their certification status under the DOT guidelines.
Implications for Sleep Apnea Patients
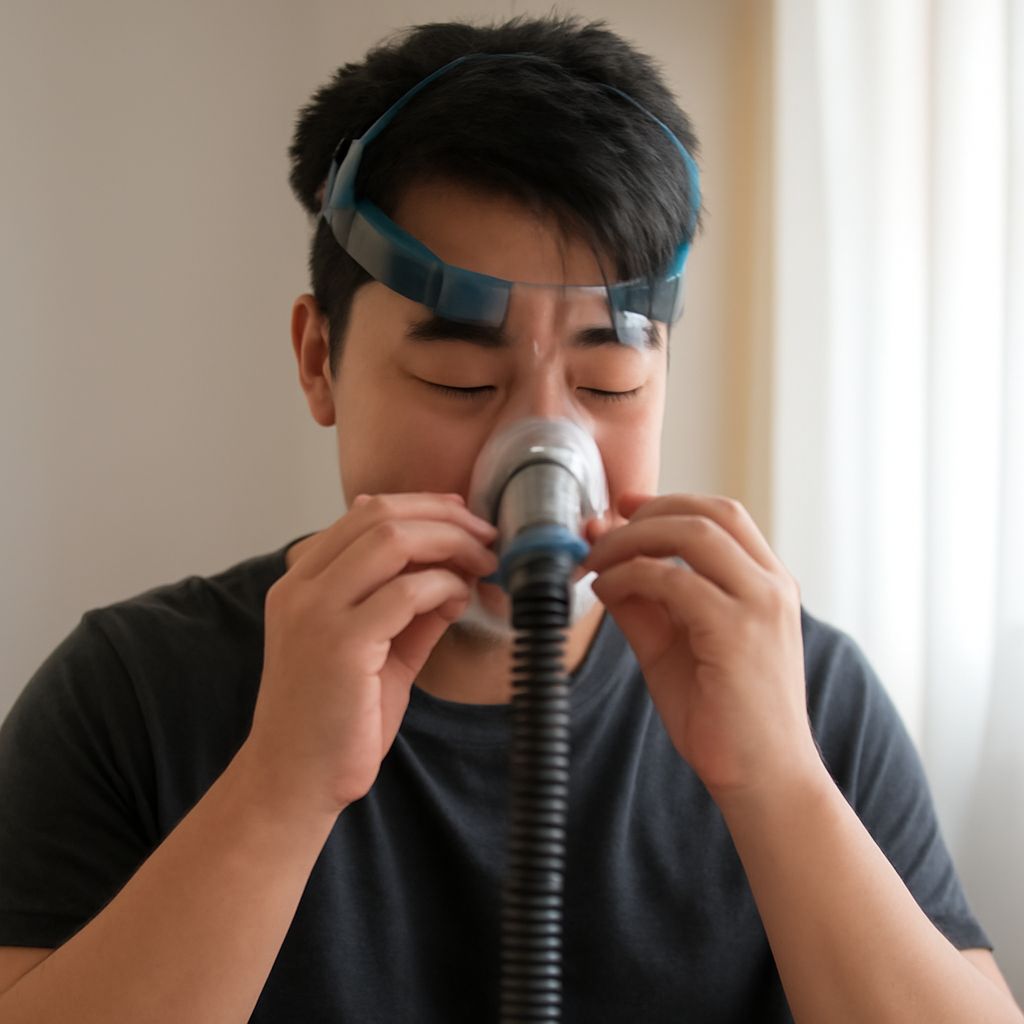
Patients diagnosed with sleep apnea will need to demonstrate effective management of their condition. This involves using CPAP machines or other treatments to mitigate symptoms. If untreated, sleep apnea can lead to severe consequences, such as brain damage over time.
For patients, complying with these new regulations not only affects their ability to maintain a commercial driving license but also their overall health. By managing the condition effectively, they can reduce risks such as brain fog and memory loss.
The Impact of Sleep Apnea on the Brain
How Sleep Apnea Causes Brain Damage
Sleep apnea brain damage is a significant concern for medical professionals and patients alike. The condition can cause interruptions in breathing during sleep, leading to reduced oxygen supply to the brain. Over time, this can result in damage to brain cells and other cognitive impairments.
Research indicates that untreated sleep apnea can contribute to structural changes in the brain. These changes may manifest as white matter lesions, which are closely related to cognitive decline. The severity of the damage often correlates with the frequency and duration of apneic episodes.
Connection Between Sleep Apnea and Brain Fog
One of the less talked about but equally disruptive effects of sleep apnea is brain fog. This symptom is characterized by feelings of confusion, forgetfulness, and lack of focus. The correlation between sleep apnea and brain fog is linked to the repeated interruptions in sleep cycles, preventing the brain from getting the restorative rest it needs.
Addressing sleep apnea effectively can lead to improvements in these cognitive functions. By adhering to treatment plans, individuals can alleviate brain fog and enhance their mental clarity and daytime functioning.
Addressing Concerns: Does Sleep Apnea Cause Memory Loss?
Sleep apnea memory loss is a legitimate concern for many individuals suffering from this condition. The chronic disruption of sleep can affect the hippocampus, the area of the brain responsible for memory formation and retrieval. Over time, this can lead to noticeable memory deficits.
While not all patients with sleep apnea will experience memory loss, the risk increases with the severity and longevity of the condition. Effective treatment and management are crucial in preventing these adverse outcomes and promoting cognitive health.
Key takeaways: The new DOT sleep apnea regulations emphasize health and safety by highlighting the significant risks of untreated sleep apnea, such as brain damage and memory loss. Understanding these implications and adhering to treatment can help mitigate these effects, ensuring better health outcomes for those affected.