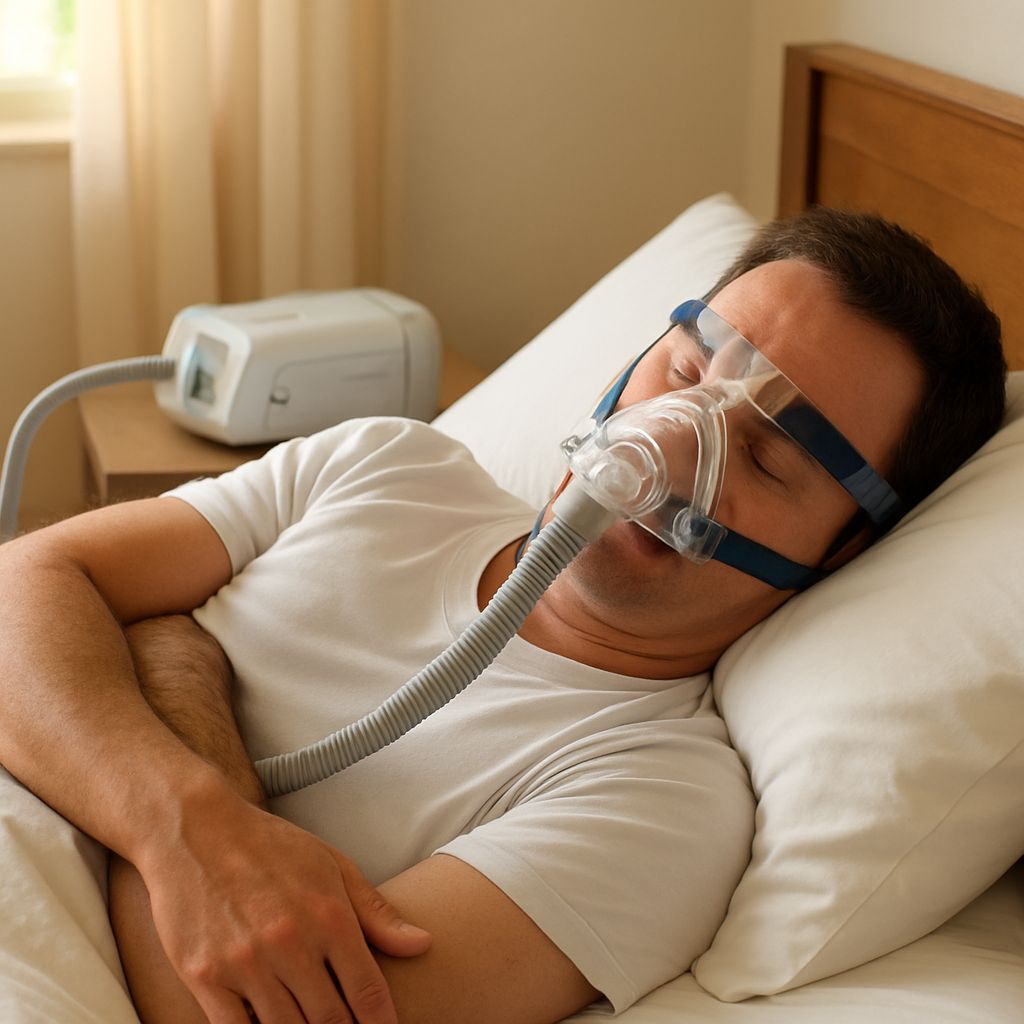
Sleep Apnea Surgery Cost, Success Rates, and Non-Surgical Options
Sleep apnea surgery cost varies between $3,000 and $10,000 for the most common procedures, with uvulopalatopharyngoplasty (UPPP) typically ranging from $6,000 to $10,000 before insurance. The financial commitment alone makes it worth understanding which surgical options actually work, what the evidence says about success rates, and whether non-surgical alternatives might achieve similar results at lower cost and risk.
Positional sleep apnea, sleep apnea chest pain as a complication, interest in didgeridoo sleep apnea training, and the question of sleep apnea surgery success rate all reflect different points on the same decision spectrum. Surgery is one option, not the inevitable endpoint of failed CPAP therapy. Positional sleep apnea, where events cluster predominantly in the supine position, often responds to behavioral intervention alone. Sleep apnea chest pain points to cardiovascular involvement that makes the case for treatment more urgent regardless of which form it takes.
Surgical Options and Their Success Rates
UPPP, the most commonly performed sleep apnea surgery, achieves surgical success (defined as 50% reduction in AHI with a final AHI below 20) in approximately 40–50% of cases at 12 months. Sleep apnea surgery success rate data for UPPP drops further at long-term follow-up, with 10-year remission rates below 25% in most series. Maxillomandibular advancement, which repositions the jaw forward, achieves success rates of 75–90% but requires 6–8 weeks of restricted jaw movement during recovery.
Hypoglossal nerve stimulation (the Inspire device) shows the highest long-term success rate among available surgical options at 68% reduction in median AHI at 5 years. Sleep apnea surgery cost for Inspire implantation runs $30,000–$40,000 before insurance, though Medicare and most major insurers cover it for qualifying patients who have failed CPAP. The selection criteria are narrow: BMI below 32, AHI between 15 and 65, and a confirmed non-concentric airway collapse pattern on drug-induced sleep endoscopy.
Positional Therapy for Position-Dependent Apnea
Positional sleep apnea, or position-dependent OSA, accounts for approximately 56% of obstructive sleep apnea cases. Position therapy devices, vibrating positional trainers worn at the back of the neck, reduce supine sleep time by 80% and lower AHI by 50–70% in confirmed positional cases. The cost is $150–$300, the risk is negligible, and the treatment effect appears within the first night. Testing for positional apnea takes one home sleep study with position recording capability.
Non-Surgical Alternatives Worth Considering
Didgeridoo sleep apnea training targets the same upper airway muscles that surgical approaches address, without anesthesia or recovery time. A 2006 Swiss study found that four months of daily didgeridoo practice reduced AHI by 23% and daytime sleepiness scores by 31% in patients with moderate apnea. The mechanism is pharyngeal dilator muscle conditioning. The effect is real but modest, suitable as an adjunct rather than a primary intervention for moderate-to-severe disease.
Sleep apnea chest pain driven by nocturnal oxygen desaturation and repeated arousals responds quickly to any effective therapy, surgical or not. The cardiovascular pathway from untreated apnea to elevated blood pressure and arrhythmia is documented in longitudinal cohort data across multiple countries. Effective AHI reduction, by whatever means, measurably lowers morning blood pressure within 4–6 weeks of consistent therapy.