CPAP Titration: What the Sleep Study Finds and How to Use Results
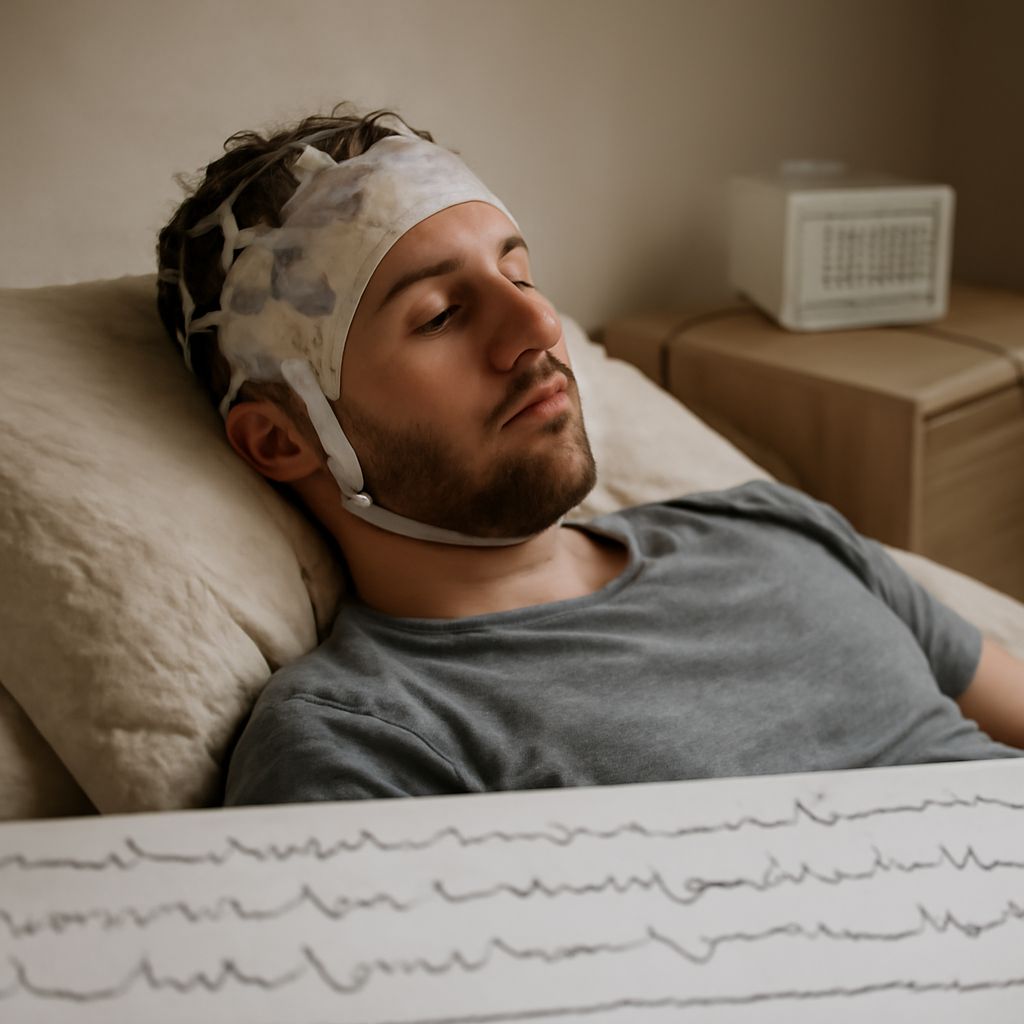
CPAP titration is the process of determining the minimum effective pressure that eliminates apnea events, hypopneas, and flow limitations during sleep. A titration sleep study accomplishes this in a monitored lab setting where a technician adjusts pressure in real time while the patient sleeps—typically increasing by 1 cm H2O increments and holding each level for 5–10 minutes to assess AHI response. The phrase “i sleep” better at a specific pressure is what the titration is designed to confirm objectively rather than through guesswork. Some patients face the decision of should i sleep or study the night before a scheduled titration, particularly students who worry about artificially poor sleep quality in the lab; the answer is that partial sleep deprivation actually increases apnea event frequency, making titration data more reliable, not less. Whether to sleep or study depends on the individual’s priorities, but canceling or delaying titration is rarely advisable when untreated apnea carries its own cognitive cost.
How a Titration Study Works
The study begins with a standard diagnostic setup: EEG leads, eye movement sensors, chin EMG, chest and abdominal effort belts, pulse oximetry, and airflow thermistors. The CPAP mask is fitted before lights out, and a brief leak test confirms the seal. Starting pressure is typically set at 4–6 cm H2O, below therapeutic range, to establish a baseline of untreated breathing events.
The technician observes the data feed from an adjacent room and increases pressure when three or more obstructive events occur within a 10-minute window. This continues through all sleep stages, with the goal of achieving an AHI below 5 events per hour in REM sleep—the most challenging stage for apnea control because muscle tone is lowest. REM usually appears 90–110 minutes after sleep onset, so adequate total sleep time matters; labs schedule 8-hour windows to ensure sufficient REM exposure.
At the conclusion, the titration report shows the pressure required for optimal control—called the 90th percentile pressure or P90. This becomes the starting prescription for an APAP machine or the fixed setting for a standard CPAP. The report also shows residual AHI at that pressure, leak rate, and the breakdown of event types.
Using Titration Results at Home
Download therapy data from the CPAP machine at 30 days and compare the home AHI to the lab AHI. Home environments differ from lab conditions in temperature, mattress type, alcohol consumption, and sleep position distribution—all of which affect apnea frequency. An AHI below 5 at home confirms the titration pressure is appropriate.
If home AHI exceeds 10 events per hour despite consistent mask use, schedule a follow-up with the prescribing provider. Common causes include pressure drift (the prescribed pressure is no longer adequate as weight or anatomy changes), new nasal obstruction from seasonal allergies, or mask leak exceeding 24 L/min, which prevents pressure from reaching therapeutic levels at the airway.
An APAP set to the titrated range—typically P90 minus 2 cm to P90 plus 2 cm—handles most night-to-night variation without requiring repeat titration. Re-titration is typically scheduled every 3–5 years, or sooner if AHI rises above 10 consistently despite proper equipment use and mask fit.